The different types of periodontal disease to know
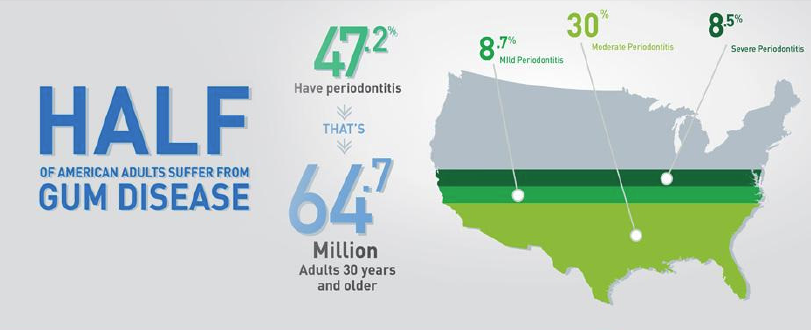 Periodontal disease or gum disease is one of the most widespread diseases and the leading cause of adult tooth loss. According to a CDC report, nearly half (46%) of all adults aged 30 years or older show signs of gum disease.
Periodontal disease or gum disease is one of the most widespread diseases and the leading cause of adult tooth loss. According to a CDC report, nearly half (46%) of all adults aged 30 years or older show signs of gum disease.
You may never develop gum disease if you are blessed with the right genes. However, some people are more vulnerable because of many factors.
There are two main types of periodontal disease: gingivitis and periodontitis. They occur differently depending on the bacteria involved, oral hygiene habits, and immune system response.
Gingivitis
Gingivitis is the initial stage of periodontal disease, where the inflammation is limited to the gum. The most common triggering factor is the accumulation of plaque and the infiltration of harmful bacteria in the gum.Other types can also cause the same clinical symptoms known as non-plaque-induced gingivitis. They are not related to bacterial plaque but involve other factors, including certain drugs, injuries, allergies, tumors, and autoimmune diseases.
The good news is that gingivitis is reversible after improving your oral hygiene. But, untreated, it can progress to irreversible periodontitis.
The most common types of gingivitis are:
Plaque-induced gingivitis
After a few days without brushing, bacterial plaque builds up on your teeth and gums. Some of it will spread beyond the gum line and trigger your immune system.Blood vessels will swell to carry nutrients and immune cells needed for self-defense, resulting in red, swollen and bleeding gums.
Gingivitis and general infections
Some infections can affect our gums and lead to gingivitis. These infections can be of bacterial origins such as syphilis, viral such as the human herpes virus, or fungal such as oral candidiasis.They lead to painful gingivitis with small sores all around the mouth. They are often associated with fever and swollen lymph nodes.
Gingivitis and injury
Sometimes gingivitis can be triggered by an injury or trauma, especially when you brush your teeth aggressively or when food debris, such as a piece of popcorn, gets stuck between the teeth and irritates the gums.Gingivitis due to autoimmune diseases
In some autoimmune diseases, such as Pemphigus Vulgaris and Mucosal Pemphigoid, antibodies made by the body attack its gum tissue.Symptoms include painful ulcerations that develop slowly. The lesions may get better or worse. But usually, they are persistent and chronic.
Drug-induced gingivitis
Some medications, such as nifedipine, phenytoin, and cyclosporine can cause gingival overgrowth.Swelling makes the gums more susceptible to inflammation, which leads to gingivitis.
Gingivitis due to allergy
Certain foods, ingredients, and hygiene products can trigger allergic reactions in some people. It usually manifests itself as diffuse red lesions, ulcerations, and a stinging or burning sensation. If you think you are allergic to a product, stop using it or replace it with another product.Periodontitis
If left untreated, gingivitis can develop into periodontitis leading to severe tissue destruction.Periodontitis is the result of the interaction of many factors. It depends on specific bacteria that can invade and destroy our tissues.
Other factors, such as smoking, stress, systemic diseases, and certain drugs, can worsen or accelerate the disease by strengthening harmful bacteria and weakening our immune system.
Different types of periodontitis can occur. The most common are:
Aggressive periodontitis
Aggressive periodontitis represents 5% to 15% of periodontal diseases. It most often affects young people, but can also occur in the elderly.It is characterized by rapid and severe destruction of the tissues surrounding the tooth.
People with aggressive periodontitis have good overall health, and the severity of the disease does not depend on the amount of plaque or tartar. In other words, it is possible to have a slight accumulation of plaque on the gums while having significant bone destruction, which explains the involvement of genetics.
Chronic periodontitis
It is the most common type of periodontitis and accounts for 95% of all affected patients. It begins between the ages of 30 and 40, following untreated gingivitis.Plaque builds up and progresses to the tissues surrounding the tooth, causing the space between the tooth and the gum to widen, forming what is known as periodontal pockets
These pockets constitute a reservoir of aggressive bacteria and inflammatory products and are inaccessible to dental brushing. Untreated, they will continue to progress deeper, leading to bone loss. Meanwhile, the gums recede, and the teeth become loose and may eventually fall out.
Unlike aggressive periodontitis, the chronic form evolves slowly, and bone destruction occurs at long intervals.
Periodontitis as a manifestation of systemic diseases
Certain systemic diseases can weaken the immune system and impact the progression of periodontal disease.Periodontitis related to systemic diseases looks like aggressive periodontitis in terms of progression and severity. They are usually associated with severe gum inflammation and virulent bacteria.
Among the systemic diseases that can cause periodontal disease:
- Blood disorders: Diseases such as Neutropenia, Leukemia, or Agranulocytosis, can disrupt the immune system and lead to severe gingivitis and periodontitis.
- Genetic disorders: Some hereditary syndromes such as Down, Papillon-Lefevre, and Histiocytosis can lead to severe periodontitis.
- Metabolic disorder: Certain diseases that affect the body's metabolism, such as diabetes, can affect your periodontal condition. In diabetes, hyperglycemia will stimulate the production of inflammatory products responsible for periodontal destruction, affect immune cell function and disrupt gum healing.
Necrotizing periodontal disease
Necrotizing periodontal disease is an acute and painful infection of the tissues surrounding the tooth. It includes necrotizing gingivitis and necrotizing periodontitis, depending on the tissues affected.They are caused by virulent bacteria and a poor immune response. They have a rapid and brutal onset, leading to intense pain, gum ulceration and halitosis.
ThNecrotizing periodontal disease may be limited to a few teeth or spread to the entire mouth. The general condition may also be affected, causing fever and swollen lymph nodes.
Among the factors that predispose to necrotizing periodontal disease:
- Stress: A high level of stress will lead to a dysfunction of the immune system resulting in a higher susceptibility to necrotizing periodontal disease.
- Smoking: Smoking is among the most significant risk factors for periodontal diseases. It alters immune cell function, decreases blood flow to the gums, and has a toxic effect on the cells that regulate our periodontal tissues.
- Immune deficiency: Studies have shown a strong correlation between temporary or long-lasting immune deficiency and the frequency of necrotizing periodontal disease. Patients with AIDS, blood disorders, and those on immunosuppressive therapy are more susceptible.
- Local factors: Factors that lead to bacterial buildups such as poor oral hygiene or poorly fitting dental crowns can promote the onset of necrotizing periodontal disease.
Factors that increase the risk of periodontal disease
Many factors can interact with the bacteria in your mouth and lead to periodontal disease.Some people have gingivitis and may never develop periodontitis. While others, genetically predisposed, are more prone to severe periodontitis.
Among the aggravating factors of periodontal disease:
- Poor oral hygiene: Poor oral hygiene will lead to the accumulation of plaque and tartar on the teeth and gums, considered the primary cause of periodontal disease.
- Systemic disease: Untreated systemic diseases such as diabetes, blood disorders, or hormonal imbalance can aggravate and accelerate the periodontal disease.
- Stress: Stress increases the inflammatory products in the bloodstream responsible for periodontal destruction and weakens our immune cells. As a result, people under stress have more severe forms of periodontal disease.
- Smoking: Tobacco contains about 4000 toxic elements for the body. It alters immune cell function and decreases blood flow to the periodontium, which can worsen periodontal disease.
- Nutrition: Nutrition can impact dental plaque formation and composition. An extreme diet can weaken our immune system and worsen bone loss.
- Medication: Some medications can cause gingival overgrowth and aggravate gingivitis.
- Saliva: Saliva plays an important protective role. It covers all surfaces of the mouth to lubricate and protect them from injury and contains antimicrobial agents that prevent bacteria from invading our tissues. Certain factors such as oral breathing and medications can decrease salivary secretion and thus increase the risk of periodontal disease.
- Teeth grinding: Teeth grinding causes excessive stress on the teeth. This will apply tension in the periodontal tissues causing tooth mobility and aggravating bone loss in periodontal disease.
- Teeth crowding: Teeth crowding will promote plaque accumulation by making some areas inaccessible to brushing. This will increase inflammation and thus aggravate the periodontal disease.
The most common symptoms of periodontal disease
Depending on the type of periodontal disease, different symptoms may occur, among them:- Receding gums: receding gums are a sign of periodontal destruction. It exposes the teeth roots causing sensitivity to cold.
- Inflamed gums: Inflamed gums are red, swollen, and bleeding. These signs exist in both gingivitis and periodontitis. Only, in the latter, they are more pronounced.
- Abscessed gums: The formation of an abscess and the drainage of pus through the tooth indicates a severe form of periodontal disease. It usually means rapid and severe bone loss.
- Teeth shifting: After losing bone, teeth will be looser and will tend to shift gradually. You may feel that your bite is not like it used to be.
- Tooth mobility: Tooth mobility means that more than one-third of the bone has been lost.
- Tooth loss: This is the final stage of periodontal disease. The tooth is held in place by a small amount of bone and will fall out.
Treatment of periodontal diseases
The treatment of gingivitis and periodontitis consists first of eliminating the cause.The first treatment goal is to improve your oral hygiene. Your dentist or hygienist will recommend additional tools such as interdental brushes or oral irrigators.
He or she will perform supragingival scaling to remove plaque and tartar above the gum line, considered the main factors of periodontal disease.
This step aims to inform and motivate you about the importance of your oral hygiene. It will help reduce the bacterial load in your mouth and get you as close as possible to the treatment plan.
In gingivitis, the initial stage of gum disease, this step is usually enough to reverse it. However, regular appointments for check-ups will be necessary.
In periodontitis, where the deep tissues are affected, including bone, ligament, and cementum, a deep dental cleaning is needed. It aims to clean the areas inaccessible to dental brushing.
Once the causes are removed, the disease stops, and the tissues begin to regenerate.
In more severe cases of periodontitis, deep periodontal pockets and bleeding gums persist even after deep cleaning. A surgical cleaning is therefore indispensable.
It consists of opening the gums and removing the diseased tissue. After a thorough cleaning, the gum will be closed with sutures to ensure healing.
This approach allows reaching areas under the gums that regular deep cleaning cannot.
In case of significant bone loss and receding gums, surgical techniques can help regenerate and restore the damaged tissue.
Prevention
Plaque is composed of different bacteria that establish connections between them to survive and increase their pathogenic factor.You can prevent gingivitis and periodontitis by maintaining good oral hygiene. Done regularly, it prevents plaque from building up and causing gum disease.
Prevention also helps reverse gingivitis and prevent it from turning into periodontitis. Good oral hygiene habits include:
- Brush your teeth two times a day for at least three minutes with a good brushing technique and a soft-bristle toothbrush to avoid hurting your gum. Brushing helps remove up to 70% of plaque.
- Floss your teeth once a day. Flossing removes 30% of the remaining plaque between your teeth. You can also use an interdental brush if your teeth are not tight. Oral irrigators can also be effective. A study has shown that oral irrigators may reduce gum inflammation.
- Learn about antibacterial treatments. If you're especially vulnerable to gum disease — for example, because of a medical condition — your dentist may recommend special antibacterial mouth rinses or other treatments to help cut down on harmful bacteria in your mouth.
- Stop smoking. Smoking is a risk factor for gum disease. Quitting smoking will improve your periodontal health.
- Take care of yourself. Some diseases and conditions harm gum health, especially diabetes, viral infections such as HIV, and hormonal disorders.
